Post Traumatic Stress Disorder and Depression — How They Connect
March 10, 2026 | By Evelyn Reed
Trauma doesn't just leave marks on your memory. It can reshape the way you feel every single day — draining your energy, clouding your mood, and making it hard to find pleasure in things that once mattered to you. If you've been carrying both the weight of a traumatic experience and a persistent heaviness that feels like depression, you may be dealing with two conditions that often travel together. Post traumatic stress disorder and depression share a complicated relationship, and understanding it is the first step toward finding clarity. In this guide, you'll learn how PTSD and depression overlap, where they differ, what treatment options exist, and how a tool like the DASS-21 online self-assessment can help you begin reflecting on how you've been feeling. This content is for educational purposes and is not a substitute for professional evaluation.

What Is the Link Between PTSD and Depression?
Post traumatic stress disorder and depression are separate diagnoses, yet they appear together far more often than most people expect. Research suggests that roughly half of those diagnosed with PTSD also meet the criteria for major depressive disorder. That overlap is not a coincidence — it points to deep biological and psychological ties between the two conditions.
How Trauma Can Trigger Both Conditions
A traumatic event can activate both PTSD and depression simultaneously. When the nervous system stays in a prolonged state of threat response, the emotional toll can extend beyond flashbacks and hypervigilance. Over time, that sustained stress may erode mood, motivation, and hope — key elements of depression.
However, the relationship also works in the other direction. If someone already lives with depression, the emotional resources they have for coping with a traumatic event may be reduced. As a result, they can be more susceptible to developing PTSD after an overwhelming experience.
Shared Risk Factors and Bidirectional Vulnerability
Several factors increase the chance of both conditions developing:
- A personal or family history of depression or anxiety
- Childhood adversity or repeated exposure to stress
- Severity and duration of the traumatic event
- Limited social support following the experience
- Pre-existing difficulty with emotional regulation
Because these risk factors overlap so heavily, it's common for PTSD and depression to reinforce each other once they appear. One condition can worsen symptoms of the other, creating a cycle that feels hard to break without support.
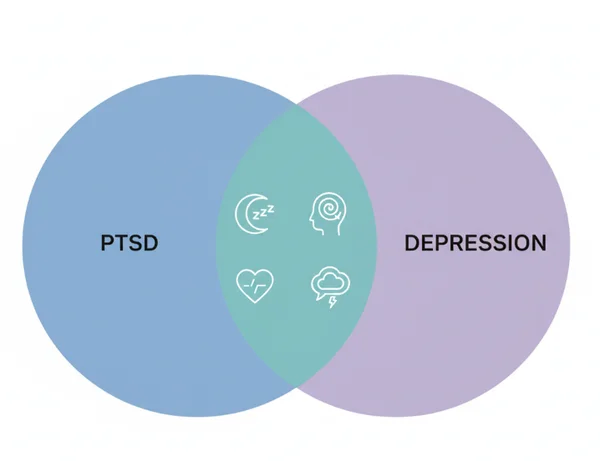
What Symptoms Do PTSD and Depression Share?
The symptom overlap between post traumatic stress disorder and depression is one of the main reasons these conditions are so frequently confused — and so frequently present together.
Sleep Problems, Concentration, and Emotional Numbness
Both PTSD and depression can disrupt sleep. You might find yourself lying awake for hours, waking frequently, or sleeping far more than usual without feeling rested. In parallel, concentration often suffers. Tasks that once felt automatic — reading, following a conversation, making decisions — may require significant effort.
Emotional numbness is another pattern that appears in both conditions. You may feel detached from people you care about, or notice that emotions seem muted — as though you're watching your own life through glass.
Negative Thoughts, Guilt, and Social Withdrawal
Persistent negative thinking is a hallmark of both PTSD and depression. These thoughts may focus on self-blame, guilt about the traumatic event, or a bleak view of the future. For some people, this leads to withdrawal from friends, family, and activities — not because they don't care, but because engaging feels overwhelming.
When these patterns stack up, it becomes harder to tell where one condition ends and the other begins. That ambiguity is itself a signal worth paying attention to.
How PTSD and Depression Differ in Key Ways
Although PTSD and depression share common ground, they are not the same condition. Recognizing the differences matters — particularly because effective support may look different depending on what you're experiencing.
Flashbacks, Avoidance, and Trauma-Specific Responses
PTSD is anchored to a specific traumatic event or a series of traumatic experiences. Its most distinctive features include:
- Intrusive memories or flashbacks — vivid, involuntary re-experiencing of the trauma
- Nightmares directly tied to the traumatic event
- Active avoidance of reminders — people, places, sounds, or situations that evoke the memory
- Hypervigilance — a heightened state of alertness, as if danger could reappear at any moment
These trauma-specific responses set PTSD apart from depression. They are directly linked to the event and tend to intensify around triggers or reminders.
Persistent Sadness Without a Single Triggering Event
Depression, by contrast, does not require a single triggering event. While trauma can certainly contribute to depression, the condition can also develop gradually from a combination of genetic predisposition, chronic stress, loss, or significant life changes.
Key features more specific to depression include:
- Persistent sadness or emptiness that lasts for weeks or months
- Significant fatigue and loss of energy even with adequate rest
- Changes in appetite or weight that are not intentionally driven
- Feelings of worthlessness or excessive guilt not necessarily tied to a specific trauma
- In severe cases, recurring thoughts of self-harm
Understanding these differences is a useful starting point — but in practice, both sets of symptoms can exist in the same person at the same time.
What Does Complex PTSD With Depression Look Like?
Not all trauma is a single event. For people who have endured prolonged or repeated trauma — especially during childhood — the resulting condition may be better described as complex PTSD, or C-PTSD. When depression accompanies complex PTSD, the picture becomes more layered.
How Chronic Trauma Shapes Complex PTSD
Complex PTSD typically develops from ongoing situations such as childhood abuse or neglect, domestic violence, captivity, or prolonged exposure to war. Unlike standard PTSD, which often traces back to one identifiable event, C-PTSD reflects the accumulation of repeated overwhelming experiences. The effects tend to be pervasive — touching identity, relationships, and emotional regulation in deeper ways.
Emotional Dysregulation and Persistent Depression
People with complex PTSD and depression may experience:
- Intense mood swings that are difficult to predict or manage
- A chronic sense of emptiness or shame that goes beyond typical depressive sadness
- Difficulty trusting others, even in safe relationships
- A fragmented sense of identity or self-worth
- Persistent difficulty controlling emotional reactions — either under-responding or over-responding
When depression co-occurs with C-PTSD, it may feel less like a distinct episode and more like a constant undertone. Professional support is especially important in these situations, because the patterns are often deeply ingrained.

How Depression, Anxiety, and PTSD Connect to Each Other
Many people searching for information on post traumatic stress disorder and depression are also dealing with anxiety. These three conditions form a triangle that frequently appears together — and for good reason.
Trauma activates the body's stress response, which includes both fear (anxiety) and emotional shutdown (depression). When the nervous system cannot fully process and recover from what happened, anxiety may settle in as chronic worry or panic, while depression emerges as withdrawal and low mood.
Some common patterns in this three-way overlap include:
- Racing thoughts combined with fatigue and helplessness
- Avoiding social situations due to both fear and lack of motivation
- Physical symptoms such as muscle tension, headaches, and digestive problems alongside emotional numbness
- Difficulty knowing whether what you're feeling is anxiety, depression, or a response to unresolved trauma
If all three feel familiar, that information can help guide a more targeted conversation with a professional.
How Are PTSD and Depression Treated Together?
Because PTSD and depression share so many features, treatment approaches often address both conditions at the same time. Working with a mental health professional can help you find the right combination.
Trauma-Focused Therapies — CPT, PE, and EMDR
Trauma-focused psychotherapy is typically the first-line treatment for PTSD, and research shows these approaches can also reduce depressive symptoms:
- Cognitive Processing Therapy (CPT) helps you re-evaluate and restructure thoughts related to the trauma — especially patterns of self-blame and hopelessness that feed both PTSD and depression.
- Prolonged Exposure (PE) involves gradually and safely confronting trauma-related memories and situations, reducing avoidance and the emotional charge around them.
- Eye Movement Desensitization and Reprocessing (EMDR) uses guided eye movements to help the brain reprocess traumatic memories, which can ease both intrusive memories and related mood disturbances.
Medication Options Often Discussed
Selective serotonin reuptake inhibitors (SSRIs) — such as sertraline and paroxetine — are among the most commonly prescribed medications for PTSD and may also help with depressive symptoms. In some cases, serotonin-norepinephrine reuptake inhibitors (SNRIs) are considered.
Medication decisions are highly individual. What works for one person may not suit another, and a prescribing professional can help weigh the options based on your specific needs and history.
Why Integrated Treatment Matters
Treating only one condition while the other remains unaddressed can limit progress. For example, untreated PTSD may continue to trigger depressive episodes even after depression is managed with medication. Integrated treatment that targets both conditions simultaneously tends to produce better long-term outcomes.
Additional supportive practices — such as regular physical activity, structured sleep habits, mindfulness exercises, and strong social connections — can complement formal treatment.
How a Self-Assessment Can Help You Reflect on Your Well-Being
If you've read this far, you may be wondering where you stand. Before reaching out to a professional, some people find it helpful to organize their thoughts through a brief self-assessment. This is not about labeling yourself — it's about gaining a clearer picture.
A self-assessment is not a diagnostic tool. It cannot replace a professional evaluation, and its results should be understood as a reflection of recent patterns — not a clinical conclusion.
What a Self-Assessment Can and Cannot Tell You
A well-designed self-assessment can help you:
- Identify which emotional patterns have been most present over the past week or two
- Distinguish between stress, anxiety, and depressive feelings
- Gather language to describe what you've been experiencing — which can be genuinely useful if you decide to speak with a professional
What it cannot do is provide a diagnosis, predict your condition, or tell you what treatment you need. It is a starting point for self-reflection, nothing more.
Using the DASS-21 as a Starting Point for Self-Reflection
The DASS-21 is a widely used, scientifically validated questionnaire that measures three dimensions — depression, anxiety, and stress. It takes about three minutes, and your results are immediate and confidential.
If you'd like to reflect on how you've been feeling lately, the DASS-21 can help you organize those thoughts in a structured way. It's free, private, and designed to give you a starting point — not an endpoint.
When to Reach Out for Professional Support
Understanding the connection between post traumatic stress disorder and depression is valuable — but reading about it is not the same as getting personalized support. Consider reaching out to a mental health professional if:
- Your symptoms have lasted more than two weeks and are getting worse
- You're avoiding places, people, or activities that are important to you
- Sleep, appetite, or concentration have shifted significantly
- You've noticed thoughts of self-harm or feel like things won't get better
- Your daily functioning — work, relationships, or self-care — has been affected
You don't need to have a diagnosis before seeking help. A professional can help you sort through what you're feeling, determine whether PTSD, depression, or both are involved, and build a plan tailored to your situation.
If you're in crisis, contact a licensed crisis service or emergency line in your area. Support is available, and reaching out is a sign of strength — not weakness.
As a first step, you can also explore the free DASS-21 assessment to reflect on your recent emotional patterns before your first appointment.
Frequently Asked Questions
Can you have both PTSD and depression at the same time?
Yes. Roughly half of people diagnosed with PTSD also meet criteria for major depressive disorder. The two conditions frequently co-occur, and having both tends to increase symptom severity compared to having either one alone.
What are the overlapping symptoms of PTSD and depression?
Shared symptoms include sleep disturbances, difficulty concentrating, emotional numbness, loss of interest in activities, negative thinking, feelings of guilt, and social withdrawal. These overlaps can make it hard to distinguish between the two conditions without professional evaluation.
What is the difference between PTSD and depression?
PTSD is directly linked to a traumatic event and involves flashbacks, nightmares, avoidance behaviors, and hypervigilance. Depression may develop without a specific traumatic trigger and is characterized by persistent sadness, fatigue, changes in appetite, and feelings of worthlessness.
What does complex PTSD and depression look like?
Complex PTSD results from prolonged or repeated trauma and often includes emotional dysregulation, chronic shame, difficulty trusting others, and identity disturbance. When combined with depression, it may appear as a persistent low mood interwoven with intense emotional swings and relational challenges.
How to treat PTSD and depression together?
Evidence-based approaches include trauma-focused therapies like CPT, Prolonged Exposure, and EMDR, along with medications such as SSRIs. Integrated treatment that addresses both conditions simultaneously tends to produce the best long-term outcomes. A mental health professional can tailor a plan to your needs.
When is it important to reach out for professional support?
Consider seeking help when symptoms persist for more than two weeks, interfere with daily functioning, or include thoughts of self-harm. You do not need a diagnosis to reach out — a professional can help you understand what you're experiencing and guide you toward appropriate support.